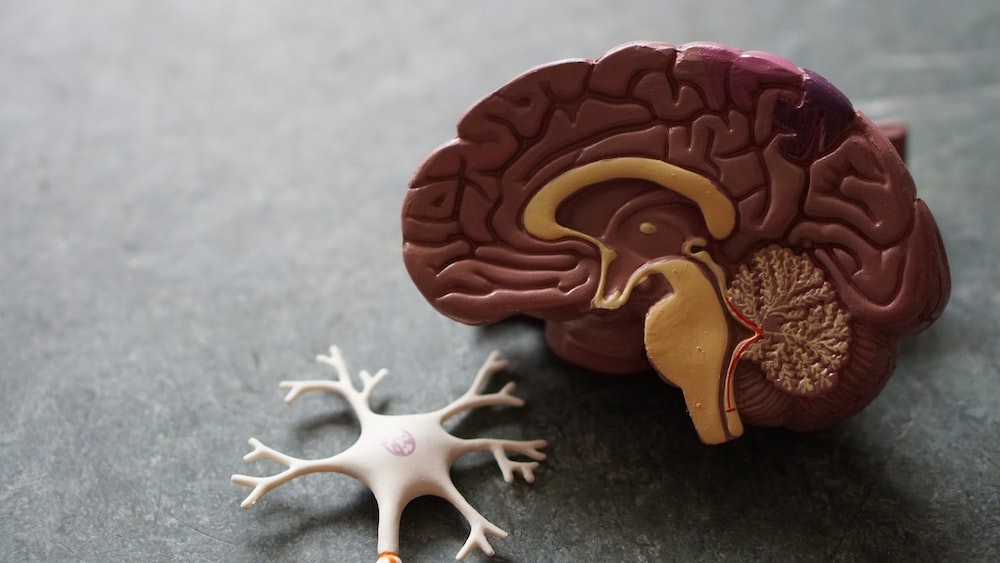
Reduced cerebral blood flow causes vascular dementia, which damages brain cells and impairs cognition. Stroke, high blood pressure, and diabetes may cause this dementia, the second most prevalent after Alzheimer’s.
Vascular dementia symptoms vary by origin and brain region. Furthermore, memory loss, focus and concentration issues, and linguistic and spatial awareness issues are prevalent. It may not be easy to diagnose, requiring cognitive, imaging, and blood testing. This page discusses the phases, kinds, risk factors, causes, symptoms, and diagnosis of vascular dementia.
Table of Contents
- Types of Vascular Dementia
- Vascular Dementia Causes:
- Vascular dementia symptoms
- 7 Stages of Vascular Dementia
- How is vascular dementia diagnosed?
- Conclusion
Types of Vascular Dementia
1. Multi-infarct dementia (MID):
Stroke-related multi-infarct dementia is the most common form of vascular dementia. Consecutive mild strokes cause brain damage and cognitive decline. Depending on the number and severity of strokes, several symptoms of MID may manifest. Memory problems, an inability to solve problems, and mood and behavior shifts are still prevalent symptoms.
2. Strategic infarct dementia:
A specific area of the brain injury that results in dementia from a strategic infarct is a form of vascular dementia. Planning, deciding, and problem-solving are all organizational processes in this part of the brain. Strategic infarct dementia is characterized by cognitive impairments such as impaired attention and focus, impaired judgment, and language and memory impairments.
3. Subcortical Vascular Dementia:
Damage to the small blood arteries in the brain’s subcortical regions, essential for processing information and directing movement, leads to vascular dementia. Motor control issues, mood and behavior shifts, and inability to focus and remember are among the symptoms that may accompany subcortical vascular dementia.
4. Binswanger’s Disease:
A rare type known as subcortical leukoencephalopathy (Binswanger’s disease) results from white matter damage in the brain. The white casing facilitates communication between the various regions of the brain. Memory loss, language trouble, and mood and behavior changes are some cognitive deficits that may result from damage to this region.
5. Mixed dementia:
When Alzheimer’s disease and vascular dementia coexist, the result is a condition known as “mixed dementia.” Memory loss, trouble focusing and paying attention, and issues with language and spatial awareness are some cognitive deficits that might result from this mix. Depending on the area and extent of the brain injury, mixed dementia may manifest in various ways.
6. Cortical Vascular Dementia:
Damage to the blood vessels in the brain’s cortex is a rare cause of cortical vascular dementia. Memory, language, and sense are located in this part of the brain. Memory and language problems, mood and behavior changes, and perception problems characterize cortical vascular dementia.
7. Post-stroke dementia:
Dementia that develops after a stroke is a subtype of the more common vascular dementia. Memory loss, an inability to focus, and issues with language and orientation in space are all indications of dementia after a stroke. People who have had several or severe strokes are more likely to develop dementia in the years following their stroke.
Vascular Dementia Causes:
1. High Blood Pressure:
Hypertension, or high blood pressure, increases vascular dementia risk. Hypertension causes cerebrovascular injury and decreased brain perfusion. Memory, attention, focus, language, and spatial awareness impairments may emerge from the occurrence above.
2. Atherosclerosis:
Lipid deposits in artery walls cause atherosclerosis, which narrows blood arteries and reduces brain perfusion. Amnesia, difficulty focusing, mental processing, and language and spatial understanding might occur from vascular dementia. Hypertension, high cholesterol, and smoking often cause atherosclerosis.
3. Diabetes:
Diabetes inhibits glucose control. Hyperglycemia-induced vascular injury may reduce brain perfusion and cerebrovascular function. Amnesia, persistent attention, mental clarity, and language and spatial understanding may come from the condition, as mentioned earlier.
4. Stroke:
When cerebral blood arteries are blocked or ruptured, cerebral perfusion decreases, and the cerebral parenchyma is injured. Strokes may induce cognitive impairment and cerebral hypoperfusion, which increases the risk of vascular dementia. Vascular dementia is more likely in stroke survivors.
5. Cardiovascular Disease:
Coronary artery disease, heart failure, and vascular dementia are connected. Cardiovascular illness may reduce brain blood flow, causing memory loss, concentration challenges, and language and visual disorders.
6. Smoking:
Smoking increases the risk of developing vascular dementia due to atherosclerosis and vascular damage in the brain. The risk of stroke rises, and stroke is a known contributor to vascular dementia.
7. High Cholesterol:
Elevated cholesterol levels can potentially induce atherosclerosis, a pathological condition characterized by the constriction of blood vessels and consequent impairment of cerebral blood circulation. The situation above may result in cognitive deficits such as compromised memory, sustained attention and focus challenges, and language and spatial perception difficulties.
8. Age:
Given the increased possibility of getting the illness, growing older is a key risk factor for the beginning of vascular dementia. The aging process may lead to the blood vessels in the brain deteriorating, which can reduce cerebral perfusion and result in cognitive deficiencies.
Vascular dementia symptoms
The signs and symptoms of vascular dementia may alter over time depending on the underlying cause and the affected area of the brain.
1. Memory loss:
Memory loss, especially in the short term, is one of vascular dementia’s most prevalent symptoms. People could have trouble remembering recent discussions, names, and events. Additionally, they could struggle to learn new facts.
2. Difficulty with attention and concentration:
Vascular dementia patients may have problems focusing, making it challenging to maintain their attention on chores or follow discussions.
3. Problems with language:
Vascular dementia patients may have trouble speaking, including choosing the right words or comprehending long phrases. Additionally, they could struggle with reading and writing.
4. Spatial awareness:
Vascular dementia patients may struggle with spatial awareness, making navigating their environment challenging or carrying out activities like driving that call for spatial awareness.
5. Organizational and planning challenges:
Vascular dementia patients may struggle with planning and organizing, making it challenging to finish activities involving many phases or stick to a timetable.
6. Mood swings:
Depressive, anxious, and irritable mood changes are all possible in people with vascular dementia.
7. Personality changes
Apathy, a lack of initiative, and diminished motivation are some examples of personality changes that people with vascular dementia may encounter.
8. Impaired judgment:
It may be challenging for people who have vascular dementia to make judgments or solve difficulties due to their poor judgment.
9. Gait and balance changes:
Vascular dementia patients may notice changes in their stride and balance, making it challenging to walk or stand for long periods.
The intensity and progression of the disease symptoms might change over time. Furthermore, the symptoms of persons who have recently had a stroke or similar medical event may sometimes alter suddenly. If you or a loved one exhibits these signs, see a medical expert to get a clear diagnosis and the best course of treatment.
7 Stages of Vascular Dementia
The stages of vascular dementia can be divided into seven distinct stages.
Phase 1: Absence of Cognitive Impairment
In the initial phase of vascular dementia, the individual exhibits no cognitive impairment. At this stage, the person exhibits no symptoms of the ailment and demonstrates specific cognitive abilities. Similarly, the potential subject under consideration may indicate factors, including hypertension, diabetes, or a previous medical record of cardiovascular illness. Likewise, effectively managing the risk factors associated with vascular dementia is crucial for individuals to reduce the probability of developing the condition.
Phase 2: Mild Cognitive Impairment
Mild cognitive impairment (MCI) represents the second stage in the progression of vascular dementia. During this phase, individuals may encounter cognitive alterations, such as challenges in recollecting recent occurrences, difficulties in lexical retrieval, and struggles with tasks that necessitate multiple stages. The modifications in question may be inconspicuous and invisible to the individual and their relatives. Nevertheless, these symptoms could manifest more prominently in the context of a cognitive evaluation.
Phase 3: Initial Phase
The initial phase is commonly referred to as the third stage. During this phase, individuals tend to encounter more prominent cognitive alterations, such as challenges with memory retention, attention span, and problem-solving capabilities. Individuals may encounter difficulties with language, such as experiencing challenges in selecting appropriate vocabulary during verbal communication. Furthermore, individuals may undergo alterations in their emotional state, such as symptoms of depression or anxiety.
Phase 4: Mid-Stage
The mid-stage is identified as the fourth phase. During this phase, the individual’s cognitive decline intensifies, necessitating aid with routine tasks such as personal hygiene and dressing. Similarly, spatial orientation may confuse familiar places. Indifference, irritation, and restlessness may also occur.
Stage 5: Moderate-Advanced Stage
The moderate-advanced stage is recognized as the fifth stage of vascular dementia. At this point, the person’s cognitive deterioration is severe, which might lead to poor speech and the inability to carry out basic daily tasks like eating. In addition to needing assistance with all everyday chores, some people may also develop incontinence. People could also have delusions or hallucinations.
Stage 6: Severe Stage
The severe stage represents the sixth and final stage of vascular dementia. At this juncture, the individual’s cognitive decline is markedly severe, potentially resulting in confinement to a bed and an inability to communicate. Individuals may also encounter seizures or other neurological manifestations.
Stage 7: End-of-Life Stage
The final stage of vascular dementia is the terminal stage. Furthermore, at this stage, the individual is nearing the culmination of their lifespan, and their physiological and cognitive deterioration is profound. Unresponsive individuals need continuous care. Furthermore, individuals may encounter various symptoms, including but not limited to discomfort, respiratory distress, and infectious conditions.
How is vascular dementia diagnosed?
The diagnosis of vascular dementia typically involves a comprehensive medical assessment, encompassing a physical examination, cognitive assessments, and imaging procedures conducted by healthcare professionals.
1. Medical history:
The healthcare professional will inquire about the individual’s medical history, encompassing prior medical ailments, surgical procedures, and prescribed medications. Furthermore, the healthcare provider may inquire about dementia in the patient’s family history.
2. Examination of the physical state:
The healthcare professional will conduct a comprehensive physical assessment to evaluate the potential presence of any underlying pathological conditions contributing to the current symptoms. The process may entail evaluating physiological indicators, such as neurological condition, heart rate, and blood pressure.
3. Assessments of cognitive abilities:
Healthcare professionals may administer cognitive assessments to evaluate an individual’s memory, attention, language, and spatial awareness. The evaluations that could be issued are the Mini-Mental State Exam (MMSE) or the Montreal Cognitive Assessment (MoCA).
4. Imaging Tests:
Imaging tests are diagnostic tools used in medical settings to visualize the body’s internal structures. MRI and CT scans may detect brain vascular blockage or damage. Lastly, the observation of these assessments may aid in determining the precise location and extent of cerebral injury.
5. Blood Tests:
Blood tests can be a diagnostic tool to detect potential comorbidities, such as hypercholesterolemia or diabetes mellitus, which may augment the susceptibility to vascular dementia.
6. Neuropsychological testing:
Neuropsychological testing may fully analyze cognitive capacities. Cognitive assessments may include memory, attention, language, and executive function tests.
7. EEG:
Brain electrical activity can be measured using an electroencephalogram (EEG). The current assessment can identify aberrant cerebral operation associated with the onset of vascular dementia.
In certain instances, the determination of this disease may rely on a fusion of these assessments and the symptomatic presentation of the individual. Likewise, supplementary examinations may be required in certain cases to eliminate alternative medical ailments contributing to the presented symptoms. It is difficult to diagnose since its symptoms might be mistaken for other dementias, and various underlying disorders can affect its appearance. Imagine you or a loved one has dementia. If so, consult a doctor immediately for a correct diagnosis and treatment.
Conclusion
Vascular dementia is a degenerative condition that poses challenges in its management. Similarly, the framework of the seven stages of vascular dementia facilitates comprehension of the disease’s progression and the anticipated developments as it advances. Managing risk factors and seeking medical attention is crucial for individuals with risk factors for vascular dementia who experience cognitive changes. Lastly, Prompt identification and intervention may aid in decelerating the advancement of the ailment and enhancing the individual’s standard of living.